The newborn phase is the make it or break it phase of breastfeeding.
It is also the most difficult.
You have a small time window to figure out how to breastfeed because your milk supply and ability to support your baby exclusively depends on it.
It’s a race between the breast and the bottle.
That is why preparing yourself for what to expect those first few weeks is so important!
I wish I had prepared myself.
If I didn’t have the amazing support network that I was blessed to have, I wouldn’t be breastfeeding my baby today.
Don’t be like me, take all the tips and advice you can get!
I have compiled a list of 14 must-know breastfeeding tips for the first 14 days that can help ensure that your newborn successfully breastfeeds.
These are the 14 tips I wish I knew about before I gave birth to my baby as I either learned about them well into my breastfeeding journey or along the way.
BEWARE this post is long as I wanted to make sure that I included ALL the information you need to know about breastfeeding your newborn baby.
If you would like to save it for a later read or reference then Pin it for later!

Disclosure: I have included affiliate links to products that I have used and enjoyed. These are for your convenience. I do receive compensation without any increase to your own price.
1. Breastfeed Within the Golden Hour

The “Golden Hour” is a term that refers to the first hour after a baby is born.
It is recommended that immediately after a baby is born, and once the baby is deemed stable, that mom and baby have at least an hour of uninterrupted skin-to-skin contact (1).
This is especially stressed if the mother intends on breastfeeding as it is oftentimes critical to success.
In this Golden Hour, the baby will instinctively attempt to latch.
It’s quite an incredible and emotional process to witness!
Newborns can recognize the unique smell of their mother’s milk, allowing them to find the nipple and then latch on and suckle (2).
In fact, there are stages of the entire process of this “Magical Hour” (3).

Stage 1: The Birth Cry
Welcome to your new world!
This is the first cry of your newborn immediately post-delivery as a consequence of lung expansion. It has been noted that this doesn’t always occur (4).

Stage 2: Relaxation
In other words, momma and baby cuddle session.
Once your newborn stops crying, they relax exhibiting minimal to no mouth or hand movements. At this stage, skin-to-skin is also initiated while a warm towel covers your baby.

Stage 3: Awakening
Hello dearie!
Usually 3 minutes after birth your baby will start to move their head, mouth, and even shoulders while opening their eyes.

Stage 4: Activity
And the emotional journey begins!
Watching especially this part gets me so teary-eyed!
It’s just such a beautiful experience!
About 8 minutes after birth you will notice increased mouthing and suckling movements as your newborn’s rooting reflex initiates.
At this stage you newborn, “keep [their] eyes open, look at [your] breast, salivate, move [their] hand to their mouth and breast, protrude [their] tongue, look at [you the] breastfeeding individual, massage [your] breast with a hand, rub [their] cheek against and / or lift their torso from breastfeeding individual’s chest.” (4)

Stage 5: Rest
A baby’s gotta rest.
Throughout the first hour, your newborn will go between intermittent stages of activity and rest

Stage 6: Crawling
The destination is reached!
About 35 minutes after birth your baby reaches the nipple through bursts of leaping, sliding, and/or crawling (4).

Stage 7: Familiarization
This is when your baby gets to know your milk machines!
Usually 45 minutes after birth, your newborn will “get familiar” with your breast by licking, touching, and/or massaging it for about 20 minutes.
Your newborn will continue to do what they did in the “Activity” stage and may even start making sounds or look around (4).

Stage 8: Suckling
Hooray!
The first official breastfeeding session has begun!
About an hour after birth (it could take longer if you received anesthesia during labor) your baby will take your nipple, self-attach, and start suckling.
You can help your newborn by ensuring that they are calm, supported, have space for their jaw to move and nose to breath, and have a deep enough latch (you can help by making a “sandwich” out of your breast, touching their top lip, and only allowing a latch when their mouth is opened wide enough) (5).

Stage 9: Sleep
All that hard work gets a restful reward.
Usually, for about 1.5 to 2 hours your newborn (and maybe even you!) will drift to sleep after their first filling meal.
This is why this first hour is so important to breastfeeding success!
It is when the bond and the confidence between you and your newborn is established.
Missing this window can make breastfeeding a little bumpier (I know because I didn’t have the ideal “Golden Hour”).
In addition to being important to the establishment of breastfeeding, immediate (within the “Golden Hour”) skin-to-skin, as with breastfeeding, is also incredibly beneficial to both the baby’s and the mother’s health (4)!
So remember, in the first-hour post-labor, plan for immediate skin-to-skin and breastfeeding.
Skip the newborn bath and tell the family to hold off!

Related Post: Things I Wish I Knew BEFORE Labor
2. If You Can, Try to Avoid Pacifiers and Bottles Until Breastfeeding is Established

Mothers will often hear this when they’re preparing their hospital plan or after they have delivered and state their desire to breastfeed.
The American Association of Pediatrics (AAP) recommends no pacifiers (or bottles) until breastfeeding is established, at around 1 month (5).

Artificial Nipples Can Cause Nipple Confusion
Pacifiers (like bottles) cause breastfeeding difficulties because of a phenomenon known as nipple confusion, although this is definitely up for debate (7).
Some believe that it’s in the design of the nipple and that plastic bottles and pacifiers don’t resemble the actual breast and confuse the baby when they’re reintroduced to the breast, and so that’s where the confusion arises.

Personally, I have witnessed something that would confirm this in my own baby as she had trouble taking certain pacifiers and bottle nipples since she was breastfed.
Sucking on a plastic pacifier or bottle nipple is different from sucking on an actual nipple, and some mothers feel their babies struggle with latching after they suck on a pacifier or bottle nipple.
However, naturally, the breast is actually easier to latch onto than any rubber nipple (which is tougher), by far, so usually, babies can go easily from pacifier to breast to bottle to breast.

Pacifiers Suppress Hunger Cues
It has also been shown that offering babies a pacifier before establishing breastfeeding suppresses hunger cues and thereby reduces breastfeeding time which can negatively affect mom’s milk supply (6).
Suckling comforts some babies to the point that they don’t even notice they are hungry.
This is especially bad in the early weeks as your baby needs to nurse often in order to build up your supply.

Incorrect Bottle-Feeding Can Cause Nursing Strikes
Incorrect bottle feeding is what causes the majority of babies refuse the breast or go on a nursing strike!
Mothers aren’t really shown the way they should bottle feed their breastfed baby.
The proper way to bottle feed a breastfed baby is upright and it is referred to as paced bottle feeding.

Here is a helpful infographic about what that looks like, but if you want more information you should check out my post “The Ultimate Guide to Feeding Your Baby Through a Nursing Strike“.

Most moms, though, tend to bottle feed their baby in a more inclined or laying position which means that their baby doesn’t have to put in much effort to get the milk flowing.
This is a problem because actual breastfeeding does require effort.
Now if you have a baby that has breastfeeding well established, this usually isn’t a huge concern and they could go back and forth without issue.
However, it is an issue if breastfeeding isn’t established and your baby is still learning to effectively remove milk from your breast.
This is why, as with the pacifier question, it is recommended to introduce bottle feeding once your baby is 4-6 weeks old (6).
Also, it is important to note that another caregiver should bottle feed baby instead of mom as this can also cause issues for either effective breastfeeding or bottle feeding.
Don’t Eliminate the Pacifier and Bottle Completely
You do want to make sure to offer the bottle (and the pacifier) before the 8 week mark or you might have a baby that rejects the bottle entirely (6).
A pacifier is also recommended in the first six months of life because it has been found to reduce the incidence of SIDS (5).
Use Your Intuition
The takeaway is to make sure that breastfeeding is established before introducing either.
However, usually, one month is a long while for parents to last without resorting to a pacifier.
I know because I used one immediately (the only way baby, and I, slept).
So, if you must use one, try to use them sparingly (I took the pacifier out once my baby was falling asleep) and properly (don’t forget about paced bottle feeding!) and you should be fine!

Related Post: The Ultimate Guide to Feeding Your Baby Through a Nursing Strike.
3. Get Lots of Skin to Skin

Immediate skin-to-skin post-delivery is essential to breastfeeding success.
In a systematic review, researchers highlighted that immediate skin-to-skin increased breastfeeding duration and success, as opposed to babies that were swaddled immediately post-delivery (8).
Another study found that disruption or delay in skin-to-skin may negatively affect not only a baby’s ability to self-latch and breastfeed effectively but also the bond between mother and baby (9).
Other benefits of skin-to-skin for babies include (10):
– Reduced risk of major infection in low birth weight newborns.
– Reduces their pain, calming them and helping them cry less.
– Releases a hormone that relieves their stress and stabilizes their breathing rate, heart rate, temperature, and blood sugar.
– Boosts their immune system, protecting against illness and disease.
– Boosts their mental development as they experience a range of smells, sounds, and textures.
– Facilitates their weight gain.
– Helps them sleep better because they are less stressed.
– Strengthens their bond with caregivers.
Benefits of skin-to-skin for mom include (10):
– Releases a hormone that helps lowers her stress and promotes her healing.
– Helps her colostrum production.
– Promotes breastfeeding by building her milk supply.
– Lowers her risk of a postpartum disorder.
– Allows mom to rest with her baby on her chest.
– Strengthens bond with baby.

Skin to skin has a lot of benefits for both baby and mom which is why it’s recommended well beyond the newborn stage.
So, although it’s very essential at the start of your breastfeeding journey, it continues to be just as essential in its progression, especially if your baby goes on a nursing strike.
Related Post: Ways To Reduce Your Baby’s Risk for Obesity
4. Take Care of Your Nipples Religiously.

Trust me on this one, your nipples will need a lot of extra care and attention immediately when you begin breastfeeding.
If your baby wasn’t as effective at self-latching in the golden hour, the latch might take a lot more time, effort, and patience.
This will mean that your nipples will take the brunt of the beating as your baby learns to breastfeed effectively.
You can avoid excessive pain by taking care of your nipples before they become damaged.
Ways to Prevent/Reduce Nipple Pain
- In order to reduce the amount of pain you might later endure, lather on the nipple cream liberally, after every feeding.
- Another common trick is to cover your nipple with expressed breastmilk and then to allow your nipples to air dry, however, this method of healing isn’t advised if you suspect that you have thrush or a yeast infection as this could actually make it worse (12).
- You can also use Soothies to alleviate nipple soreness. They feel amazing on sore nipples! Definitely an essential for breastfeeding!
Related Post: Body-Shock: 11 Things No One Tells You About Your Post-Delivery Body

5. Don’t Neglect the Latch.

You have probably heard this before, but effective breastfeeding is really all in the latch.
Neglecting the latch is a common mistake new moms make because they just get tired of the breaking and relatching cycle with an increasingly frustrated baby.
However, not correcting the issue will lead to more problems in the long run.
Consequences of Incorrect Latch
A shallow latch means that your baby isn’t adequately nursing or removing milk from your breast, which means that your baby will feel tired before they are full.
A common side effect is longer nursing sessions and fewer breaks in between sessions (not to be confused with cluster feeds which we will touch on later).
This is both exhausting for baby and mom!
Also, a bad latch means nursing pain and nipple damage because usually, bad latch implies that your baby is gumming on the nipple directly instead of massaging it to get milk out.
You don’t want to neglect this as your breastfeeding can become a very painful experience, something it shouldn’t be.
How to Get a Good Latch

A good latch will appear deep with your baby’s lips flared outward and will not hurt for mom.
If you feel a pinching sensation while breastfeeding, immediately break the latch by putting your finger into the side of your baby’s mouth and pulling outward as to break the seal.

To relatch, “sandwich” your breast with your dominant hand, touch your baby’s nose with your nipple while pulling it slightly back with your thumb, and only let go and allow a latch when your baby has opened their mouth wide enough.
Be careful not to push the back of your baby’s head when trying to bring them towards your breast as you can actually upset them this way.
Repeat until you feel a gentle pulling sensation while breastfeeding.
This infographic does a great job showing the difference between a good and a bad latch and visually demonstrates how to get a good latch.

It is important to note that a let-down can also feel like a sharp pain in the first stages of breastfeeding, however, this pain is usually centered around the armpit area.
If you find yourself struggling to successfully and painlessly latch, you might want to ask a lactation consultant to evaluate your baby for a possible tongue/lip tie.
Related Post: Breastfeeding Survival Guide: 12 Things I Wish I Knew About Breastfeeding
6. SUPER IMPORTANT!!! Look Out for Tongue and Lip Ties!

My baby had both a tongue and a lip tie, so having gone through it, I want to raise more awareness about just how essential it is to breastfeeding success.
To understand why you must know how your baby actually breastfeeds.
Why the Latch is so Important
The “latch” is how your baby establishes the suction over your nipple.
When your baby has a good latch, they are able to efficiently draw milk out of your nipple when you have a letdown.
An effective latch has two components.
First, the lips must be flared out.
Second, the tongue must extend beyond your baby’s gum line.


How Lip Ties Affect the Latch and Cause Breastfeeding Pain
A lip tie inhibits the flaring out of the lips as it is the tissue that connects the gum to the inner membrane of the top lip.
The closer the tissue is to the teeth, the more serious the lip tie, the less flare there is.
Since your baby isn’t able to flare out their lips very much and they lose suction often when attempting to breastfeed.
As a result, your baby will gum down on your nipple just to maintain a latch and nurse.
This has a lot of negative implications for breastfeeding.
For one, gumming down actually inhibits milk flow.
It’s like trying to drink something through a straw while simultaneously biting down on it.
It also makes breastfeeding extremely painful for mom as the nipple takes the brunt of the clamping down force.
This is why some moms get cracked, split, and even bleeding nipples.
Ouch!!
How Tongue Ties Affect the Latch and Cause Breastfeeding Pain
A tongue-tie inhibits the ability of the tongue to extend beyond the gum line as it is the tissue connecting the bottom of the tongue to the floor of the mouth.
Just as with the lip tie, the closer this tissue is to the tip of the tongue, the more serious the tongue tie, the “shorter” the tongue.

Now, contrary to common belief, a posterior tongue tie (when the tie isn’t considered as severe and is located more towards the back of the mouth) still has negative implications for breastfeeding since it still results in a “shorter” tongue.
When your baby’s tongue doesn’t extend beyond their gumline, this also results in the gumming of your nipple, and you’re back to inefficient nursing and nipple pain.
Consequences of Tongue and Lip Ties
I want to emphasize that when your baby doesn’t nurse efficiently, there is a cascade of side effects.
You get longer nursing sessions.
You have more frequent nursing sessions.
Your baby is always tired and cranky (they’re working really hard with little reward!) and always seems to be hungry.
Your baby loses weight instead of gaining it.
Your milk supply drops because your baby isn’t able to remove milk from your breasts effectively.
And it repeats until you are forced to supplement for your baby’s survival and well-being (fed is best!).
So, as you can see, recognizing a tongue and lip tie is SUPER important not only if you want to breastfeed, but for your baby’s health!
How to Identify a Tongue and Lip Tie
If you would like to personally check your baby, for a lip tie just lift their upper lip and check for the appearance of the frenulum or tissue.

Now the tongue-tie is a bit trickier.
However, an easy way to pinpoint tongue tie is that if your baby has a lip tie, they will almost always have a tongue tie (13)!
This is how it usually looks like.

Now, if your baby doesn’t have a lip tie and you still suspect a tongue tie because you and your baby are showing the signs of one, then it is best to seek a specialist to confirm one.
Getting a Specialist to Confirm a Tongue/Lip Tie
Most physicians are able to identify an anterior tongue tie (you could spot one immediately by just looking under a baby’s tongue), and they usually check for it post-delivery, however, a posterior tongue is more difficult to see.
A specialist will usually test your baby’s suckle instead.
To properly check for a posterior tongue tie, an experienced specialist will usually have mom lay baby on mom’s lap facing mom before looking into baby’s mouth, “upside-down”.
If the doctor or lactation consultant doesn’t do this, they don’t know how to correctly identify a tongue tie.
Go to someone else.
I had two pediatricians and two lactation consultants tell me that my baby didn’t have a tongue-tie.
Taking a friend’s advice, I sought out a tongue tie specialist and in the first consultation, they FULLY EXPLAINED how they properly check for a tongue tie and SHOWED me that my baby had a lip tie AND a posterior tongue tie.
We clipped both her lip and tongue tie that day, and although it was a tough journey, at nine months we are still going strong breastfeeding (**Update** We breastfed a full year, so definitely glad we had those clipped!)!
Related Post: Breastfeeding Problems and How to Properly Identify a Tongue and Lip Tie
7. Watch for Milk Coming In

The first “milk” that your baby consumes is called colostrum.
What is Colostrum?
Colostrum is everything your baby needs in its first days of birth as it is filled with important fats, proteins, carbs, and immune factors that support your baby’s digestion of meconium (baby’s first sticky, tarry poop), thus reducing jaundice, and strengthen their immunity against infection (14).
You start producing this thick, sticky, concentrated milk mid-pregnancy, between 12 and 18 weeks (14).
This yellow milk is everything your baby needs in its first few days of life.
The rest of your milk comes in about 2-3 days after birth, but in some cases, it may take longer than 3 days (15).
Why You Should Watch for When Your Milk Comes In
The reason why understanding this is important is that the coming in of milk, in some cases, can be sudden and can both overwhelm your baby and even your breasts.
Some babies experience feeding and behavioral changes at the breast.
Feedings can become shorter and/or less often, and vice versa.
Your baby could even flat out refuse to nurse (like in my case) which could be confused for nipple confusion when in fact it is because they have difficulty latching on due to engorgement.
What is Engorgement?
Engorgement is when your breasts become overfilled with milk due to milk being produced but not properly removed from the breast.
This can be very painful for momma.
Engorgement is very common in the first few days postpartum due to the sudden coming in of milk which can easily overwhelm a newborn baby learning to breastfeed.
If you do see that…
- your breasts still feel full after feedings, in those early days
- your baby struggles to nurse while visibly still appearing hungry after each feeding
- and/or your baby completely refuses to nurse, crying at your breast
… engorgement is definitely something to watch out for!
Your baby might be overwhelmed by the sudden influx of milk and you will need to remove milk by pumping or by manually expressing until your breasts soften.

How to Relieve Engorgement?
Heat works really well in releasing clogged milk ducts so you could either apply heat compressions during pumping or manually express while taking a hot shower, whichever works best.
Just make sure that you remove the milk or you can cause your milk production to completely stop (15).
What to do if Your Milk Comes in Later?
If your milk takes longer than 3 days to come in, consider talking with a lactation consultant to determine the cause of the delay.
Oftentimes a delay can be due to inefficient nursing, however, it can also be a consequence of birth complications (like retained placenta and use of pain medications), maternal health (like obesity and hyperthyroidism), maternal breast issues (like hypoplasia and inverted nipples), or the fact that mom is a first time mom (15).
There are steps you can take to induce milk production which include skin-to-skin, pumping, and ensuring that you offer the breast every time your baby is hungry and wants to nurse (there’s a reason newborn babies cluster feed!).
Supplementation should be avoided unless deemed essential to your baby’s wellbeing (failure to thrive or excessive weight loss).
Always pump the same amount you supplement to ensure your milk supply doesn’t drop.

Related Post: My Breastfeeding Story: How I Went from Supplementing to a 400 oz Stash in a Month
8. No More Than 10% Birth Weight Loss

Some weight loss in the first few days of life is normal for newborns.
Newborns are born with extra fluid, so it is expected that they will lose between 7% and 10% of their birth weight in correspondence to losing that fluid (16).
However, a loss of over 10% of their birth weight is a concern and could indicate that your baby isn’t breastfeeding efficiently and/or that your milk supply isn’t sufficient.
If your baby is not treated with supplementation (whether that be your pumped breast milk or formula) your baby could risk a failure to thrive.

What is a Failure to Thrive?
A failure to thrive, simply put, is when a baby’s growth falls significantly behind its peers.
This could refer to various areas of growth that range from mental and physical development to weight, and that could be the consequence of a variety of factors.
However, for an exclusively breastfed healthy newborn, more often than not, a failure to thrive is meant that the baby has lost too much weight due to issues with breastfeeding itself.
This can be extremely stressful for mom as she usually starts to doubt her milk supply and her ability to exclusively breastfeed and sustain her baby, I know because I have been there.
Regardless, a mother’s first concern is the health and wellbeing of her baby, that is why monitoring your baby’s weight is so important!

What to do if You’re Baby Loses More than 10% of Their Birth Weight?
If your baby has lost a significant amount of weight in the first few days, you must supplement to ensure that they are fed.
This does not mean that you must quit breastfeeding.
On the contrary, breastfeed ON-DEMAND and then have your partner supplement your baby with your pumped breastmilk (or formula, per physician direction) while you pump the same amount your baby consumes, to ensure that your milk supply is sustained.
Once you ensure your baby is getting fed, then you can work to identify the problem with your lactation consultant.
They will measure the amount of breastmilk your baby nurses at each breast and then determine whether there are issues with your supply or the way your baby nurses.
In my case, the problem was in the fact that my baby had a tongue and lip tie.
Catching the problem early on saved my breastfeeding experience, which is why monitoring development is so important to breastfeeding your baby, not just their well being!
Weight Loss Doesn’t Always Indicate a Failure to Thrive
I want to emphasize, though, that weight loss doesn’t always mean that your baby is failing to thrive.
If you were given a lot of IV fluids during labor, your baby’s weight could be artificially greater than if you weren’t given fluids (17).
Therefore, it really does depend on a lot of other factors other than just weight.
If your baby appears happy and healthy, if your baby is developing neurologically and physically well, if your baby’s physical and cranial (head circumference) growth is on track, and if you are not experiencing pain and difficulty while breastfeeding, then weight loss should not be a major concern.
You and your pediatrician should and probably will continue to monitor your baby’s progress, however, there’s no indication that you are not able to exclusively breastfeed and sustain your baby or should supplement with formula (17).
Also, don’t let generic growth charts discourage you either as most are based on a formula-fed baby’s growth (18).
You can get more accurate growth charts from the World Health Organization (WHO) for breastfed infant girls and boys on the Center for Disease Control (CDC) website.
Misinformation should not add to the fact that breastfeeding moms are already prone to doubting their abilities to independently nourish their babies!
Related Post: Things Every Breastfeeding Woman Needs To Hear
9. Tracking, Tracking, Tracking!
![]()
Since we are already on the topic of monitoring, I want to add that weight is not the only thing you will be monitoring in those first few months.
Immediately after you deliver you will be asked to record the amount of wet and dirty diapers you change, when your baby sleeps and how long, and when your baby nurses, which breast and the length.
Luckily there are neat apps that can easily get this done for you.
I used the iOS app called Baby Tracker and it lived up to the hype!
It definitely saved me from a lot of headaches if I had to time and write everything down myself!
So, while the app tracks your baby, you still need to know what numbers to look out for.

Tracking Diapers
Tracking your baby’s diapers lets you know if your baby is nursing efficiently.
First Week Diaper Tracking (19)
In the first week, you should expect a dirty diaper and a wet diaper for each day of life (1 on day 1, 2 on day 2, …).
By day 4, your dirty diapers will stay at a range of 3-4 stools a day.
There needs to be at least a quarter size amount of poo to be counted as a dirty diaper.
Baby’s first stool is meconium. It is dark green, tarry, and sticky.
After that clears up it should be yellowish and loose and runny but can also appear seedy.
Your baby’s wet diapers should also stay at a range of 5-6 a day once your milk comes in.
There needs to be about 3 tablespoon worth of pee (test it out on a clean diaper to know how it feels like) to be counted as a wet diaper.
If you are not using a diaper with a water sensitive strip, you can check the diaper for wetness using a tissue.
Your baby’s pee should be light, and if it is dark yellow/orange this is usually an indicator that your baby is dehydrated and therefore not nursing efficiently.
Diaper Tracking for Weeks 2 to 6 and Onward (19)
You should expect the diaper amounts to stay somewhat consistent through 6 weeks with 3-4+ dirty diaper a day and 5-6+ wet diapers a day.
After 6 weeks, though, your baby may not have as many dirty diapers (some babies stool so infrequently that they have a dirty diaper once in 7-10 days!), so just monitor their weight gain to ensure that everything is normal.
The number of wet diapers will also drop a little after 6 weeks to 4-5 a day, however, the amount of pee in each diaper will actually increase (a felt amount of 4-6 tablespoons) due to the growth of your baby’s bladder capacity.
![]()

Tracking Sleep
Tracking your baby’s sleep won’t be as complicated as tracking diapers.
You should know that although newborns sleep a lot, about 16-17 hours a day/24-hour period, they don’t sleep for long stretches, especially exclusively breastfed newborns (20)!
The average length you should expect your baby to sleep is no longer than 2-4 hours both day and night (20).
I personally would err on the shorter stretch of sleep as breastmilk is digested faster than formula.
My baby averaged 30-45 minute stretches in the day (it’s called cat-napping; it sounds horrible and it really was!) and 2-3 hour stretches at night (which was nicer but still rough).
If you also have a bad sleeper my advice is to sleep when your baby sleeps, leave the housework for a few weeks until you get back on your feet and things normalize.
Now, although frequent and fussy nursing is normal (we will discuss cluster feeding and growth spurts next), your baby should not act like this all the time.
If you have any concerns that your baby is having difficulties nursing which you believe is causing them to be always nursing and fussy, talk to your lactation consultant and have them monitor your feedings and your baby’s weight gain in case there are underlying issues inhibiting efficient nursing.

Tracking Nursing Schedule
Nursing in the newborn stage will be one of the most difficult parts of your entire breastfeeding experience.
If your baby wasn’t able to establish proper latch and breastfeeding in the “golden hour”, it might take a little more effort and patience on your part as your baby is still learning how to efficiently breastfeed (I promise the pain goes away!).
Frequent nursing and long is something to expect and prepare for in the first few weeks.
This is how your baby establishes your milk supply and reduces engorgement, especially when your milk comes in (19).
First Week Nursing Tracking
In the first week, your should expect no fewer than 10-12 nursing sessions a day with gaps no longer than 2 hours during the day and 4 hours during the evening, wake and feed your baby otherwise (19).
If your baby nurses more, that is totally fine.
There is NO such thing as nursing too much, only too little (so be aware!) (19).
Also, make sure to nurse immediately when your baby shows signs of hunger or else you will be dealing with a fussy baby that you will first need to calm before feeding.
Here is a helpful diagram of what these signs look like.

As mentioned already, don’t worry if your newborn nurses long and frequently at your breasts, in the first few weeks.
It is good to know that cluster feeding (when your baby is extra fussy and nurses constantly for several hours, especially in the evenings) and growth spurts (when your baby is also very fussy and nurses a lot for several days; notable growth spurts are on days 7-10, weeks 2-3, and weeks 4-6) are completely normal and indicate that your baby is developing well and stabilizing your milk supply for the rest of your breastfeeding journey (21)(22).
Additionally, babies also nurse for comfort (breastfeeding reduces stress and pain), mom is their safe haven, so remember that it might not be convenient but it is helping your little one adjust to their new world (22).
Let your baby finish nursing on one breast completely before offering the other one.
Nursing Tracking for Weeks 2 to 6
You should expect to continue nursing your newborn at least 8-12+ times a day/24-hour period.
Continue nursing as you did in the first week.
If your baby’s weight gain has rebounded positively, you could stop waking your baby to nurse and just nurse when your baby shows signs of hunger.
First, though, talk to your pediatrician and lactation consultant to get the go ahead.
Also, make sure to also track which breast you nursed on last so that you offer the other one in order to avoid having different sized breasts after weaning (yes, that is so a thing!)!
It can definitely seem overwhelming considering that you are probably already exhausted after labor, so you might want to recruit help, if possible.
However, tracking everything is essential to ensuring your baby is healthy and developing normally.
It is also important for making sure that everything is working well with breastfeeding.
Related Post: 27 Helpful Charts for Breastfeeding Moms
10. Make Sure that Your Baby is Actually Swallowing at the Breast

Usually, moms aren’t taught to pay attention to how effectively their baby nurses unless their baby doesn’t have adequate weight gain.
However, it is important to be aware of this in order to ensure both baby health and breastfeeding success.
If your baby will be exclusively breastfed in its first days of life, this will be absolutely crucial to their wellbeing.
How to Know if Your Baby is Actually Swallowing?
You want to make sure that they’re audibly swallowing (you might hear a soft “k” sound, or, if your baby is a quiet swallower, you will notice a pause in their breathing) and moving their chin and bottom jaw in a ripple motion after a few sucks as it will confirm that they’re getting the nutrients they need (11).
Other indications that your baby is adequately nursing, apart from weight gain and diaper counts, is if you feel a let-down when nursing, your breasts feel completely emptied out after each feed, and your baby shows signs of being full (they are alert and active after feedings) (11).
Watch Out for Your Baby Falling Asleep While Nursing
Also, you want to make sure that your newborn baby completes nursing and doesn’t fall asleep at the breast or else they could go to sleep still hungry and wake up even hungrier (and fussier!).
It is quite a warm and comfortable right next to mom’s heart, so it’s bound to happen.
If your baby does fall asleep at the breast just tickle their feet!
Better yet, you can strip your baby down to their diaper when they nurse so that they don’t warm up and get cozy too quick, and therefore stay awake and feeding longer.
If your baby is constantly falling asleep at your breast this could be a sign of an underlying nursing problem as your baby could be actually getting tired before getting full because they are nursing inefficiently.
The breast your baby nurses from should feel firm and full before the feeding and then tender and emptier after the feeding.
Regardless, watching if your baby is swallowing will help you determine whether or not your baby is nursing efficiently and will help you identify issues before they become detrimental to both your chances at breastfeeding and your babies health.

11. Make Sure to Pump

I intended on exclusively breastfeeding my baby, so I didn’t really think I would really need things like bottles and a pump.
Boy was I wrong!
Unless you want to be strapped down, you might want to consider getting both!
The pump alone, though, will go a long way for you momma!
I had no idea that pumping would be so important to my breastfeeding journey.
It helped me treat my engorgement, supplement my baby with breast milk when breastfeeding was difficult, and maintain and increase my supply.

Pumping to Relieve Engorgement
Engorgement is common when your breast milk comes in because many newborns aren’t able to remove milk fast or well enough.
Once your breasts become engorged, your baby isn’t able to latch (your nipples get very hard).
The only way to save both your milk supply and breastfeeding overall is to pump that milk out.
If you don’t pump it out, you might develop mastitis (a terribly painful bacterial infection in your breast) which causes your milk to “burn up”.
You don’t necessarily need a pump to relieve engorgement.
You could also take a hot shower and massage/hand express your milk.
Click HERE for a visual illustration of how to do this.

Pumping to Supplement
Not all newborns are great breast-feeders.
If your baby is struggling with latching or having other breastfeeding difficulties, you might have to supplement their nutrition while you figure out the problem.
Some breastfed babies are not able to digest formula well, so pumping your breast milk might be your only alternative.
Well, and nothing beats mom’s milk!
You could start by pumping after every breastfeeding session.
You want to make sure that you still work at breastfeeding before you offer supplementation.
So, once your baby nurses, pump the leftover milk out of your breasts and have your partner feed the breast milk by bottle using the paced-bottle feeding method, that way your baby is getting the nutrients it needs and your milk supply is safe.

Pumping to Maintain Your Milk Supply
If your newborn baby isn’t able to effectively empty your breasts at each feeding, your milk supply could be in jeopardy too!
Milk production is stimulated when your baby nurses by the release of oxytocin.
The emptier the breast, the greater the milk production stimulation.
That is why your milk production consequently decreases when your baby isn’t adequately breastfeeding and emptying your breasts.
This is another reason why you should pump after nursing sessions when you supplement.
Just make sure to pump out at least the same amount that your baby consumes so that your supply doesn’t drop.
You don’t want to lose your supply!

Pumping to Increase Your Milk Supply
If you are trying to increase your milk supply, you can also do so by taking advantage of this same mechanism.
Once your baby starts breastfeeding efficiently and you stop supplementing, you could continue to pump after every nursing session as you would before.
I would typically pump each side for about 15-20 minutes.
That is how I increased my supply and how I was able to create a stash of over 400 oz in one month!
You could also power pump, or pump in intervals, and increase your total supply that way.
It’s usually done to quickly increase a supply that has taken a sudden hit.
Here is how it is done.
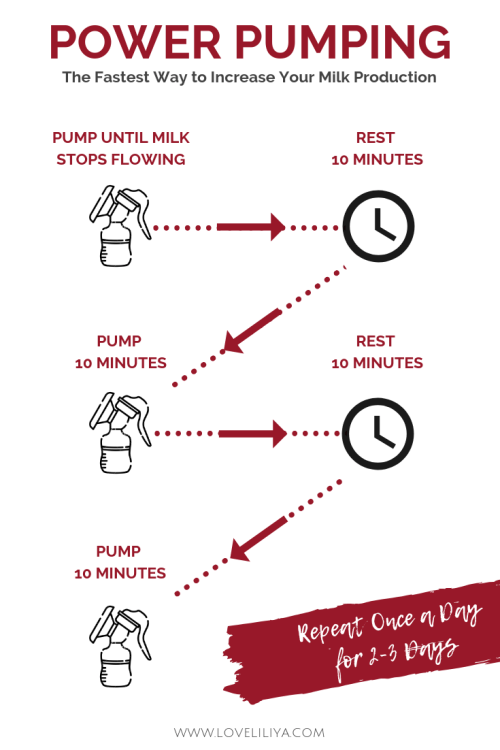
Your pump can also be used to stimulate a let-down which is super useful if your baby goes through a nursing strike and gets impatient at the breast!
DID YOU KNOW?
A let-down is initiated at both breasts at the same time?
So once milk starts flowing at the breast being nursed, it also starts leaking at the opposite breast.
Use a Haakaa to save that precious gold!
Don’t let it go to waste!
How to Get Your Pump for FREE?
Did you also know that you can get a breast pump for free?
I, personally, had no idea until a momma shared the secret with me!
That was a relief!
Have you seen how pricey those machines get?!
All you need to do to find out is to contact your insurance and ask them if you qualify for a FREE pump or if you need a doctor’s prescription to get one.
I received a decent pump from my insurance, to keep.
I was also able to get a hospital-grade Medela pump prescribed (these are literally the BEST pumps out there but they’re SUPER pricey!).
Definitely find out before you spend any of your own money!
Related Post: Clever Ways to Start Saving Money on Baby During Pregnancy
12. Prepare for Cluster Feeding

I already mentioned cluster feeding, but I really wanted to emphasize on being prepared for it.
What is Cluster Feeding?
Cluster feeding is when your baby feeds very often towards the end of the days.
To put it into perspective, my baby would bunch feed starting at around 4-5 PM and until 9-10 PM and would eat for 30 minutes at a time every 30-45 minutes.
The reason why your baby does this is to both build up your supply and to “tank up” for the night (23).
Your baby gets enough milk so that they could sleep longer stretches at night.
Babies are also naturally fussier at this time, so don’t worry too much if your baby goes through sessions of latching on and off and crying.
If your baby isn’t showing distress or pain signs like colic and if they act normally during the day, then it is totally normal (23).
As a side note, you have less milk flow (this milk is fatter so your baby is still getting needed nutrients) towards the evening, so that also adds to the fussiness.
When is Baby’s First Cluster Feed?
The first cluster feed newborns go through is usually on the second night of birth (they’re usually not as hungry on the first night since they were receiving loads of nutrients from their mom’s placenta up until delivery).
If you didn’t sleep well through your labor, birth, or after delivery, that cluster feed hits you hard. I slept what felt like a total of 10 broken hours in three days. It was EXHAUSTING!
Of course, it’s different for every baby, but every baby goes through something like it.
How Can You Prepare Yourself?
My advice is to get as much sleep as you can (sleep when your baby sleeps) and ask for help at least for that first week.
My mom came over for that second night and it was a HUGE saver because my husband wouldn’t have been able to help me as much as she had because he had just as much sleep as I did.
How Long Do Cluster Feeds Last?
Cluster feeding is terrible, especially in the first few weeks to months, but it does get better.
My baby still “tanked up” at 10 months, but she got more efficient which reduced the cluster feed length tremendously. I wouldn’t even call them cluster feeds anymore. She will just nurse through three let-downs (I alternate breasts if necessary), and then head to bed.
For most moms, cluster feeds improve around 3-4 months but it can be earlier than that, so it does get so much easier!
Other Bunch Feeds You Should Know About.

Cluster feeds/fussy evenings, improve with time, however, growth spurts are another type of fussy, bunch-feeding sessions that increase in length over time and last through the first year of your baby’s life.
These are sometimes referred to as “leaps”, coined so by the popular “Wonder Weeks” book.
Technically, growth spurts extend until the teen years, but breastfeeding moms are usually interested in their effects on the first year of their baby’s life as they are the ones that directly affect breastfeeding.

During this period babies eat more often and are fussier.
They are undergrowing both physical and developmental milestones which can be stressful for them (24).
They nurse more often to increase mom’s milk supply to compensate for their growth.
Babies typically undergo growth spurts in the first few days after birth (contributing to cluster feeding), Days 7-10, Weeks 2-3, Weeks 4-6, Month 3, Month 4, Month 6, and Month 9 (24).
Every baby is different so use this as a reference, not a guide.
Related Post : My Top 5 Useful Apps for First Time Moms
13. Try to Have Baby Sleep in the Same Room as You

Having your baby sleep in the same room is both comforting and convenient for both mom and baby.

You and Your Baby Need the Proximity
Your baby needs to be near you especially in the first days of their life.
Separation from the womb was a pretty traumatic experience for them, and their new world is cold, loud, and frightening.
You are their shelter and protection, their warmth and security.
You also need to be close to your baby as the physical separation at birth was just as traumatic for you.

Breastfeeding at Night is Easier
Second, having your baby nearby makes it so much easier to breastfeeding at night and then after to quickly put them to bed.
This is really convenient when you are up 3 to 4 times at night!
It really does save time and energy which means more sleep and rest for mom!
Sleeping in the Same Room Decreases the Risk of SIDS
Sudden Infant Death Syndrome (SIDS) is a major concern of every parent.
Having your baby sleep in the same room as you reduces their risk of SIDS in those first days of life (25)!
However, this is only true if your baby isn’t sleeping directly in your bed.
There are safe co-sleeping options like the Dock-A-Tot, I would advise consulting with your pediatrician first though, but direct co-sleeping is very dangerous.
Babies are tiny and fragile and they don’t have the strength to support themselves, sleeping in the same bed with two grown adults and adult sized bedding, among other hazards, is a serious safety concern.
Related Post: (Surprising!) Baby Registry Items I Couldn’t Super Mom Without
14. Know What to Expect (+Essentials)

Knowing what to expect seems like a vague and repetitive tip considering that we have listed a lot of tips that are aimed at letting you know what to expect and preparing you for those first few weeks of breastfeeding.
Although I know that you can’t fully prepare yourself for breastfeeding a newborn, you can get as much information as possible to help you better manage the chaos.
The more you know, the more “peace” and confidence you have in yourself and your abilities to do it.
I have dedicated an entire post to what I wish I had known before breastfeeding.
This survival guide will help prepare you for the journey!
I have also created a post on which essentials you need in order to breastfeed.

Breastfeeding is a natural process, but if there are products to make it easier then I’ll take that any day!
Related Post: 13 Breastfeeding Essentials for First-Time Moms (And How to Use Them)
Re-Cap
Breastfeeding a newborn is tough but totally possible.
These tips will definitely give you the head start in making sure you’re successful.
Your main goal, though, is to get your baby fed.
Babies can’t talk to let you know if things are working out and they cry for many reasons, so you can’t rely on that entirely either.
However, there are things you can monitor to ensure that your baby is getting the nutrition they need.
Things to Watch Out For (26)
- Is your baby gaining enough weight?
- Is your baby having at least 6 wet diapers a day?
- Is your baby getting regular dirty diapers?
- Is your baby’s urine light or dark yellow/orange?
- Is your baby always fussy after feedings?
- Is your baby sleepy/tired all the time?
- Does your baby have a yellow tint to their eyes and skin?
- Does your baby spit up/throw up a lot and/or forcefully?
Although not all babies show the same symptoms when in distress, you as mom will feel that something just isn’t right.
Trust your instincts!
Talk to your lactation consultant if you have any concerns!
You got this momma!

If You Enjoyed Reading This, You Might Also Like…
- Breastfeeding Survival Guide
- How I Went From Supplementing to an Oversupply
- 27 Helpful Charts for Breastfeeding Moms
- 40+ Breastfeeding Snack Ideas for Breastfeeding Moms
Sharing is Caring
Share this with other mommas you know and care about.
We need to help and empower each other to make mom life as easy as possible so we can continue to be super moms in all the important areas!
Stay smart momma and be on the lookout for more helpful posts!
You can find more helpful information like this on my website.
Subscribe to my email list to get updates on new posts.
Better yet, follow me on Pinterest and you won’t ever miss a thing!
Until next time mommas!





